
Running a dental practice today is not only about delivering great care. It is also about getting paid on time, keeping schedules full, and making sure patients do not face surprise costs after treatment.
That is where dental credentialing becomes a major factor. When a dentist is not properly credentialed with insurance networks, claims can get delayed, reimbursements can be reduced, and even simple services can turn into billing headaches for both the front desk and the patient.
Many dental practices get delayed because credentialing moves slowly, and even one missing document can push approval back by weeks. If patients are treated while the provider is still pending, it can lead to denials, refunds, and front desk confusion. What seems like paperwork actually impacts cash flow, patient trust, and practice growth.
Dental credentialing is the process insurance companies use to confirm that a dentist is qualified to provide care and eligible to join their network. During credentialing, the payer reviews the provider’s identity, education, license status, professional history, and other key records before approving participation.
It helps payers confirm that the provider is properly trained, licensed, and in good standing. It also protects the practice because once the provider is approved, the practice can submit claims under the correct network rules and fee schedule.
Credentialing in dentistry often gets mixed up with “enrollment,” but they are not exactly the same. Credentialing is the verification step, and enrollment is the setup step that comes after approval (so your provider profile and billing can go live).
Even though each payer has its own process, most dental credentialing applications check the same core areas.
Insurance companies confirm who the provider is and whether they can legally practice.
Dental school, graduation date, specialty training, and supporting documents may be required.
Your active state dental license is essential, and if applicable, other certifications must be current.
Many payers ask for a work history, CV, and details about past affiliations.
Insurers often verify details directly with official sources (licensing boards, schools, employers, and insurers).
Credentialing itself is not about procedure codes, but being “billing ready” matters because payers expect correct documentation once you go live. For 2026, CDT updates are active and must be used correctly on claims.
Dental credentialing is not “just paperwork.” It directly affects whether your practice can grow smoothly or gets stuck in delays. Here is why it matters:
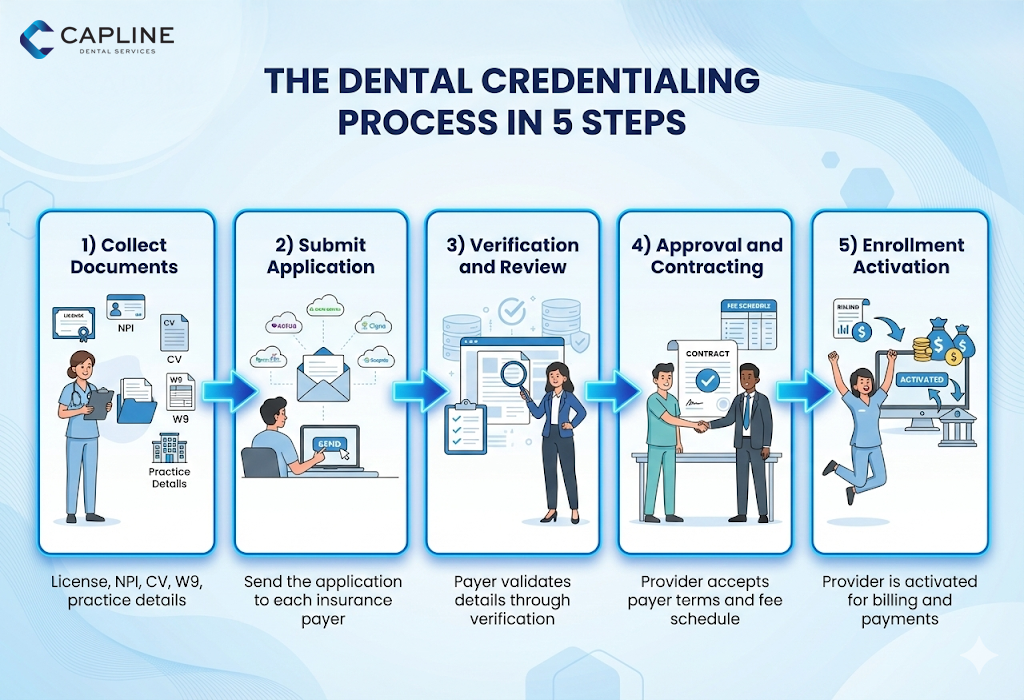
Most dental credentialing follows a predictable path, even though forms and timelines differ.
This is where many delays begin. Missing one document can set you back weeks.
You submit credentialing applications to each payer or use a shared platform when accepted.
Payers validate the information through primary source verification.
Once approved, the provider agrees to payer terms, guidelines, and fee schedules.
The payer sets up the provider record so claims and remittance can run properly.
If you are wondering how to credential a dental provider, this is the cleanest way to approach it. Below is a practical dentist credentialing checklist used by many practices to avoid rejections:
Even strong practices get stuck because credentialing has moving parts. Here are the most common reasons credentialing slows down:
Incomplete submissions: A single missing field or expired attachment can pause everything.
Multiple payer requirements: What works for one payer might not work for another, so you cannot copy and paste blindly.
Hard to reach payer teams: Some payers are quick to accept applications but slow to respond to follow ups.
Data mismatch across systems: If your license name, practice address, or NPI formatting is different across documents, payers may request rework.
Recredentialing deadlines: Credentialing is not “one and done.” Recredentialing happens on a schedule, and missing it can risk network status.
The honest answer is that it depends on the payer, how clean your application is, and how quickly verifications are completed. Dental credentialing usually takes 2 to 4 months per insurance payer. In most cases, dental credentialing is approved within 60 to 90 days, but it can take 90 to 120 days if extra verification is needed or documents are missing. To avoid delays, most dental practices should plan for 2 to 4 months per payer, especially when applying to multiple insurance networks at once.
If you want faster approvals, the goal is simple: reduce back and forth.
Incomplete submissions are a leading cause of delays, so accuracy takes precedence over speed.
Keep one master folder for each provider, containing the latest versions of all documents.
CAQH and ADA work together to make it easier to share data with dental plans for credentialing and directories.
Create a simple tracker showing submission date, status, and last follow up date.
For services performed in 2026, claims must use the correct CDT 2026 codes, so update billing workflows before the provider goes live.
When it comes to simplifying and automating the credentialing process for dental practices, these tools are known for reliability and efficiency:
If you want fewer denials and fewer delays, these best practices are worth following:
The biggest problem in credentialing in dentistry is inconsistent information across forms.
Even after approval, small changes like an address update can trigger payer issues if not updated.
Credentialing often takes months, and delays can stall revenue.
If you follow up, you want proof and dates.
Delta Dental states recredentialing can happen every three years, depending on the payer rules.
If you want dental credentialing handled correctly, with fewer delays and cleaner approvals, Capline can help you manage the full process from start to active status. Explore Capline Dental Services and get support that keeps your providers credentialed, active, and ready to bill without stress. Get in touch with our experts for a free consultation today.
A dental credentialing specialist handles the process of enrolling dentists with insurance companies and keeps their credentials updated to avoid payment delays.
Usually, an active state dental license, education proof, ID verification, and a CV are required. Specialty certificates may be required if applicable.
Aetna often accepts CAQH submissions in many states, while Delta Dental may follow its own network process and has strict recredentialing cycles.
Missing documents, expired licenses, incorrect provider details, payer backlogs, and slow follow-ups from either side.
Most insurance companies require dentists to re-credential every few years to keep their participation active.
The payer will request corrections. Once fixed, you resubmit the updated application and supporting documents.