
In a dental practice, the work does not end when the patient leaves the chair. You still have to turn that treatment into a clean claim, get the insurance payment in, and then collect whatever balance is left. That entire process is dental billing, and when it is not handled properly, things get messy fast.
You may have seen this happen in real life. The schedule looks full. Patients are coming in. The clinical work is going well. But the revenue feels slow. Payments are stuck in follow ups. Claims keep coming back for “small corrections.” Patients call the front desk asking why their balance looks different from what they were told. It is not that anyone is doing a bad job. It is that billing has many moving parts, and even one mistake can trigger delays.
This guide will walk you through what is dental billing, the real dental billing meaning in day to day practice, and show you how billing works from start to finish.
Dental billing is the process of submitting dental treatment details to insurance and collecting payment from both insurance and patients in a correct and organized way.
If you want the simplest answer to what is dental billing, it is the system that turns treatment into money. That includes checking benefits before treatment, selecting the correct procedure codes, preparing the claim, submitting it, tracking the response, fixing rejections, posting payments, and billing the patient for the remaining balance.
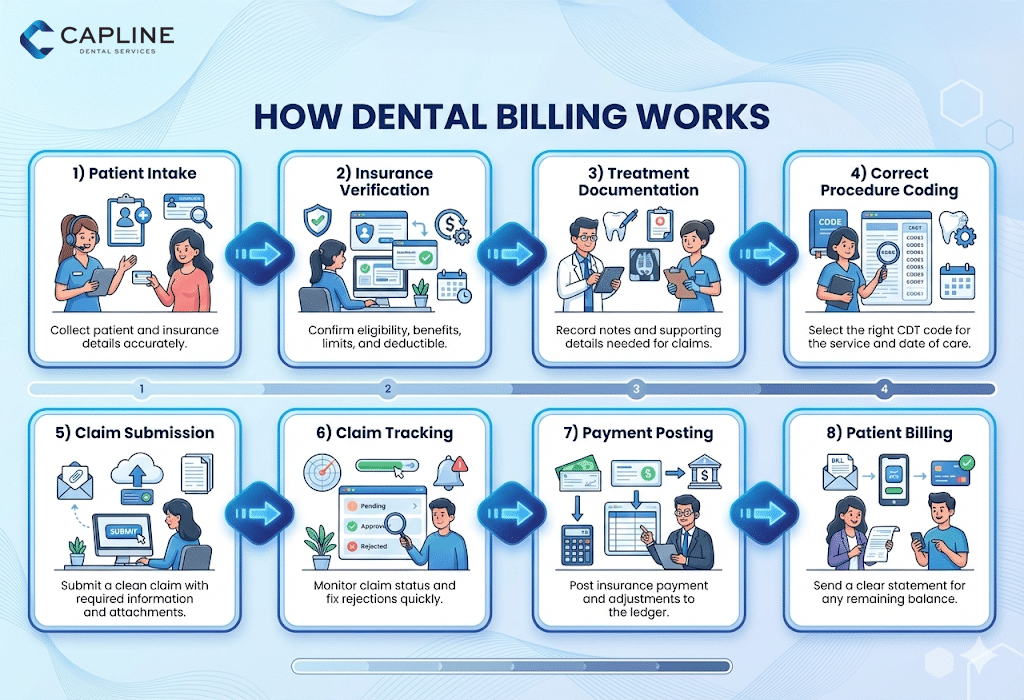
A strong dental billing workflow is not complicated, but it needs to be consistent. Most practices follow the same general flow, even if the software and insurance portals differ.
The billing process starts at scheduling, because this is where patient and insurance details are collected. This sounds basic, but it is where many claim issues begin. If the subscriber name is wrong, the policy number is incomplete, or the plan is outdated, the claim can be rejected before it even gets reviewed.
Before treatment, your team confirms eligibility and checks key plan details, like deductibles, annual maximums, and frequency limits. This step matters because it reduces surprises later. When verification is rushed, patients often assume they are covered, and then get frustrated when the insurance payment comes back lower than expected.
Capline Dental Services explains that eligibility verification is the first step of the billing process and should be done before the appointment, because it helps create clean claims, quicker payments, and a smoother billing experience.
Your clinical notes are not only for treatment history. They also support reimbursement. Some procedures require narratives, diagnostic records, or supporting details. If documentation does not match the service, the payer may delay the claim or request additional information.
Most dental plans use CDT procedure codes. In 2026, practices are expected to use the current CDT code set for dates of service in 2026. One professional coding guide clearly notes that CDT is revised annually, and effective January 01, 2026, practices are expected to use CDT 2026 when submitting claims.
Clean claim submission means the claim includes correct patient information, correct provider identifiers, correct codes, and any required attachments. When a claim is complete from the start, it is less likely to be rejected, and it is more likely to move quickly through payer review.
Once submitted, most claims go through simple statuses like submitted, accepted, rejected, pending review, paid, or denied. Tracking these statuses consistently helps your team catch problems early instead of finding out weeks later when cash flow starts feeling tight.
After a payer processes the claim, your office posts the payment, applies adjustments, and identifies what the patient owes. This step directly affects patient trust. If posting is incorrect, patient statements look confusing, and patients hesitate to pay because they do not understand the numbers.
This is one of the most common questions, especially for practices that handle procedures that may sometimes be billed through medical coverage.
Dental billing usually follows dental plan rules and dental procedure codes. Medical billing follows a different structure and often requires diagnosis support, additional documentation, and medical necessity language depending on the service.
The biggest difference is how coverage is decided. Dental plans often include annual maximums, waiting periods, and frequency limitations. Medical plans work differently and typically depend heavily on the diagnosis and clinical justification.
In practical terms, dental and medical billing are two different workflows. If a practice mixes them without a clear process, claims can become harder to track, harder to defend, and easier to deny.
Most dental billing problems are not rare or unusual. They happen every day, and the reason they hurt is because they repeat.
One of the most common issues is inaccurate insurance details. If information is incorrect at intake, the claim can get rejected immediately. Another issue is incomplete verification. When benefits are not reviewed properly, the practice may perform treatment assuming coverage, and the patient gets upset when insurance pays less than expected.
Coding errors also cause trouble. Many claims require correct code selection for the exact service performed. In 2026, staying aligned with the updated code set for the year matters, because claims should reflect the correct codes for the 2026 date of service.
Missing documentation is another big issue. Certain services often trigger payer reviews, and if an attachment or narrative is missing, the payer may request more information or delay processing.
Then there is the follow up problem. A rejected claim is often fixable, but only when it is caught early. When rejections sit untouched, they turn into older accounts receivable, and that is when cash flow starts to feel unpredictable.
Accurate dental billing is not about doing more work. It is about reducing repeated mistakes that steal time.
Start with consistent insurance verification. When every patient goes through the same verification process, your team catches issues early and avoids surprise balances later.
Next, focus on clean claim preparation. Your claim should match your documentation. Your codes should match the treatment. Your provider and location details should match what the payer has on file. When these pieces align, the claim has fewer reasons to be stopped.
Coding matters too. Your team should be using the correct CDT codes for the year of service, especially in 2026. Keeping codes current reduces avoidable rework and keeps claims aligned with payer expectations.
Claim tracking should also be steady. Not once a month. Not only when someone complains. Tracking should be part of routine operations, so issues get fixed before claims become old.
Payment posting needs the same discipline. The faster and cleaner the posting, the faster you know what insurance paid and what the patient owes.
Finally, keep patient statements simple. Patients do not want confusing billing explanations. They want clarity. A clean statement and a clear balance improve collections without creating tension.
There is no one right answer here, but there is a clear way to decide.
In-house billing works well when you have stable staff, consistent workflows, and enough time to track claims properly. It also works when claim volume is manageable and the practice is not drowning in follow ups.
Outsourcing helps when billing becomes too hard to control internally. That usually happens when claims are delaying too often, denials increase, staffing changes happen, or the front desk is doing more billing follow ups than patient support.
Some practices outsource because they want stronger consistency. Others outsource because they are growing and want billing to stay stable while clinical operations expand.
Capline Dental Services supports practices by helping them bring structure to billing and collections so claims do not keep getting stuck in the same cycle.
Instead of letting rejected and delayed claims pile up, Capline works on clean claim workflows, proper follow ups, and consistent posting so the billing process stays under control. That support makes a difference because most practices are not failing at billing. They are simply overloaded, and billing requires time and precision.
With a structured billing approach, practices typically see fewer repeated errors, better cash flow consistency, and less stress on the front desk because patient billing becomes easier to explain.
When your practice is fed up with slow payments, missing claim corrections, and patient inquiries about balances, optimizing your dental billing can render everyday operations to feel more relaxed.
A more regular billing process will assist you in collecting the money more quickly, decrease the workload, and leave the patients and the staff more at ease.
In case you would like to make dental billing seem easier and more predictable, Capline Dental Services can help manage your practice in systematized claim processing and consistent follow-up. Connect with the experts at Capline Dental Services to minimize waiting times, enhance collection, and maintain a patient-centered focus for your staff. Call us today.
The delays in claims are frequent, the refusal is rising, or your employees are no longer able to maintain follow ups.
It can be so, as there is not much room to make errors in terms of payer rules, codes, and documentation requirements.
Incorrect patient insurance information or missing required claim details.
When growth, staffing changes, or higher claim volume makes billing hard to control in house.
Coding mistakes, missing documentation, coverage limits, and benefits that were not verified before treatment.